Contents
- Summary
- Vegetarian Cohorts and Standardized Mortality
- AHS-2: Mortality (2024)
- Meta-Analysis of CVD, IHD, and Stroke (2023)
- Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial: Mortality (2023)
- Meta-Analysis of Stroke Risk among Vegetarians (2021)
- Stroke Rates of Vegetarian Health Professionals (2021)
- Stroke Risk in Taiwanese Vegetarians (2020)
- EPIC-Oxford: Ischemic Heart Disease and Stroke Incidence (2019)
- AHS-2: Cardiovascular Mortality and Protein Source (2018)
- Meta-Analysis of Mortality and Cancer (2017)
- EPIC-Oxford: Mortality (2016)
- EPIC-Oxford: Heart Disease Incidence (2013)
- AHS-2: Mortality (2013)
- Mortality Meta-Analysis (2012)
- EPIC-Oxford: Heart Disease Mortality (2009)
- Heidelberg Study (2005)
- EPIC-Oxford: Preliminary Mortality Rates (2003)
- British Mortality (2002)
- Mortality Meta-Analysis (1999)
- Adventist Health Study (1999)
- Appendix A: Excluded Papers
- Bibliography
Summary
Vegetarians (including vegans) have mostly been found to have similar mortality rates to regular meat-eaters. Vegetarians (including vegans) have been found to have a lower incidence of heart disease, and vegans, especially, have a lower incidence of type 2 diabetes (as reviewed in Type 2 Diabetes and Vegan Diets). This could indicate that vegetarians, on average, are healthier while alive but don’t necessarily live longer.
Vegetarian Cohorts and Standardized Mortality
The table below lists the main cohort studies designed to examine differences between vegetarians and meat-eaters. They recruited people with similar lifestyles but different diets.
Most of the cohorts reported a standardized mortality ratio (SMR) which is the death rate of the study population compared to the greater population of their region. The cohort SMRs show about half the mortality rate of people under age 90. The researchers attributed most of the differences to lower smoking and the healthy volunteer effect, but some may have been due to a healthier diet (Key, 1999, Key, 2009).
| Cohort Studies with Large Numbers of Vegetarians | ||||||
|---|---|---|---|---|---|---|
| Study | Country | Years | Number of Vegans | SMR | Reference | |
| Adventist Mortality | California | 1960-65 | .49 | Key, 1999 | ||
| Adventist Health | California | 1974-97 | – | |||
| Health Food Shoppers | UK | 1976-88 | .56 | Key, 1999 | ||
| Oxford Vegetarian | UK | 1981-2000 | .46 | Key, 1999 | ||
| Heidelberg | Germany | 1978-99 | .48 | Key, 1999 | ||
| EPIC-Oxford | UK | 1993 – | 2,600 | .52 | Key, 2009 | |
| Adventist Health Study-2 | USA | 2002 – | 5,500 | .67 | Fraser, 2019 | |
These cohort studies are observational. They provide both cross-sectional and prospective data to measure differences between groups made up of individuals who are self-motivated to follow particular eating patterns. Because the participants haven’t been randomized to the different eating patterns, and their diets aren’t controlled beyond a broad classification, it’s harder to determine cause and effect than for randomized clinical trials. Observational studies are more practical than clinical trials—they cost less per person and make it easier to follow people for longer periods of time which tends to be required for measuring differences in disease rates. For information on the types of nutrition studies and their pros and cons, please see Basics of Nutrition Research.
AHS-2: Mortality (2024)
In a report from Adventist Health Study-2 (Abris, 2024), 88,400 people were followed for an average of 11 years (until 2015).
Mortality rates at both age 65 and age 85 were compared using three different models. Model one corrected for sex, race, and region of residence. It showed a significant reduction in mortality at age 65 for vegetarians compared to non-vegetarians (HR 0.74, CI 0.69-0.78). Models 2 and 3 corrected for many variables, including body mass index (BMI), and found a weaker, but still significantly lower risk of death at age 65 (Model 3: HR 0.89, CI 0.83-0.95).
Unfortunately, no models adjusted for most of the typical variables, such as smoking, exercise, and socioeconomic status, without also adjusting for BMI. Because vegetarians have a lower BMI and BMI is associated with higher risks of chronic disease, adjusting for BMI might eliminate a significant benefit of a vegetarian diet.
By age 85, a lower risk for mortality for vegetarians only existed in Model 1 (HR 0.88, CI 0.83-0.94).
Vegans followed a similar pattern of a lower risk for early death in Model 1 (HR 0.88, CI 0.82-0.95) but not in Models 2 or 3. Vegan men, however, had a lower risk of early death at age 65 for all three models (Model 3: HR 0.72, CI 0.58-0.88).
When looking at specific diseases, vegans (as well as lacto-ovo-vegetarians and pescatarians) had a significantly lower risk of early death from renal failure at both ages 65 and 85. There were no other differences between vegans and meat-eaters that reached statistical significance. While vegans had much lower hazard ratios for death from diabetes (0.44 at age 65 and 0.65 at age 85), these differences didn’t reach statistical significance.
Meta-Analysis of CVD, IHD, and Stroke (2023)
Dybvik et al. (2023) conducted a meta-analysis of cohort studies examining whether vegetarians and vegans have a lower risk of incidence or death from cardiovascular disease (CVD), ischemic heart disease (IHD), or stroke.
These studies were included:
- Adventist Mortality Study
- Adventist Health Study 1
- Adventist Health Study 2
- Nurses’ Health Study 1
- Nurses’ Health Study 2
- Health Professionals Follow-up Study
- EPIC-Oxford
- Health Food Shoppers Study
- Oxford Vegetarian Study
- UK Biobank
- Heidelberg Study
- Tzu Chi Health Study
- Tzu Chi Vegetarian Study
They observed:
- A 15% reduction in the relative risk of CVD and a 21% reduction in IHD for vegetarians compared to non-vegetarians. Using World Cancer Research Fund (WCRF) criteria, they determined the overall evidence to indicate a probable protective causal association.
- No clear association for total stroke or stroke subtypes (hemorrhagic and ischemic) for vegetarians.
- An 18% reduction in the relative risk of IHD among vegans when compared to nonvegetarians, although this association was not statistically significant.
- No clear association between vegan diets and CVD or stroke, but the number of studies was small.
- That adjusting the results for body mass index (BMI) reduced the association between vegetarian diets and IHD by about one-fifth.
The researchers noted that in many of the studies the participants may have changed their diet during follow-up, which could have biased the results against a benefit of a vegetarian diet.
Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial: Mortality (2023)
The Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial cohort followed 117,673 participants for an average of 18 years (Blackie, 2023, United States). There were 329 (0.3%) lacto-ovo-vegetarians, 310 (0.3%) pesco-vegetarians, and 140 (0.1%) vegans, as determined by one Food Frequency Questionnaire at baseline. Participants only had to follow their diet for one year before baseline to be placed in their respective diet group.
Unlike most other studies, vegans had a relatively high average body mass index (BMI): omnivores (27.2), lacto-ovo-vegetarians (25.7), pesco-vegetarians (25.3), and vegans (26.9). Vegan participants also had a relatively high percentage with comorbidities: omnivores (38.9%), lacto-ovo-vegetarians (33.3%), pesco-vegetarians (30.2%), and vegans (41.5%).
In the fully adjusted model, vegans had a trend towards a higher risk of mortality: HR 1.27, CI 0.99–1.63. The authors speculated that:
The high prevalence of comorbidities and BMI in the vegan group compared with the Adventist and other previous studies, in which vegans had the lowest average BMI among the diet groups, may indicate that our self-identified vegans recently switched to a vegan diet because of health concerns.
…[T]he potentially shorter duration of following vegetarian/vegan diets might not have been sufficiently long enough for our study participants to have the typical health benefits associated with vegetarian/vegan diets.
Meta-Analysis of Stroke Risk among Vegetarians (2021)
Summary: Compared to omnivores, vegetarians have a similar risk of stroke. But they might be at a higher risk for a subcategory of stroke, hemorrhagic stroke, which is caused by bleeding in the brain.
Unnithan and Mehta (2021) report that hypertension is the most common cause of hemorrhagic stroke and that other risk factors are low cholesterol levels and low triglyceride levels, among other conditions (also see Ma, 2019; Wang, 2013; Valappil, 2012). Because some vegans have very low cholesterol levels, an increased risk of hemorrhagic stroke has been a concern.
Lu et al. (2021) conducted a meta-analysis of stroke risk among vegetarians. Combining the results of seven studies, there was no significant association for a vegetarian dietary pattern and the risk of stroke (HR = 0.86, CI 0.67–1.11). In separating the results by type of stroke, there was no significant association between vegetarian diets and ischemic stroke (HR = 0.56, CI 0.22–1.42, n=3) or hemorrhagic stroke (HR = 0.77, CI 0.19–3.09, n=2).
Only two reports in Lu et al.’s meta-analysis provided results for hemorrhagic stroke. The EPIC-Oxford study from the U.K. found a higher risk of hemorrhagic stroke for vegetarians (a group that included vegans; HR 1.43, CI 1.08-1.90). This higher risk for hemorrhagic stroke was counterbalanced by a study from Taiwan that found a lower risk in vegetarians (HR 0.34, CI 0.12-0.98); it’s not clear what percentage of vegetarians were vegan.
The lower relative risk for hemorrhagic stroke of Taiwanese vegetarians might be due to a higher risk there among the general population. Unnithan and Mehta (2021) report that the percentage of hemorrhagic stroke is 8–15% in the United States, the United Kingdom, and Australia but 18–24% in Japan and Korea. Data from 2006–2008, a timeframe that partially overlaps with the meta-analysis, show a 19% risk of hemorrhagic stroke in Taiwan (Hsieh, 2010). In 1992, Hu et al. found that hemorrhagic stroke represented 22% of all stroke cases in Taiwan. Thus, the lower relative risk of hemorrhagic stroke among Taiwanese vegetarians shouldn’t be interpreted as ameliorating the higher risk of hemorrhagic stroke among vegetarians in EPIC-Oxford.
Stroke Rates of Vegetarian Health Professionals (2021)
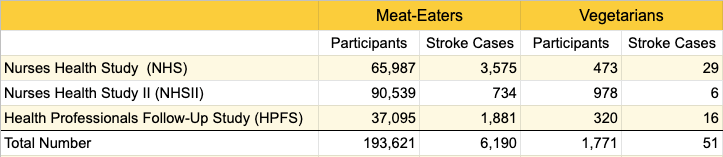
Baden et al. (2021) combined data from women in the Nurses Health Study (1984-2016) and Nurses Health Study II (1991-2012), and from men in the Health Professionals Follow-Up Study (1986-2012). Participants were resurveyed about their diet and other variables every 2 years; the number of vegetarians increased as the study progressed. Vegetarians were defined as reporting meat and/or fish intake of 0 or < 1 time per month.
Vegetarians had an insignificant trend toward a lower rate of stroke that was ameliorated with the fully adjusted model. It seems plausible that the fully adjusted model was over-adjusted, wiping out any negative impacts of eating meat.
The subtype of stroke wasn’t analyzed due to the small number of cases among vegetarians. Personal correspondence with the lead author confirmed that the adjustments were based on the most recent biennial updated information for these variables.
Stroke Risk in Taiwanese Vegetarians (2020)
A 2020 study combined two Taiwanese prospective cohorts resulting in 13,352 total participants, of whom 4,143 of were vegetarian (Chiu, 2020). After 8 years of follow-up, vegetarians had a lower risk of both ischemic and hemorrhagic stroke (Cohort 1 had 5,050 people and 30,797 years of follow-up while Cohort 2 had 8,302 people and 76,797 years of follow-up for a average of 8.06 years).
In Cohort 1, ischemic stroke was lower in vegetarians (HR 0.26, CI 0.08–0.88) and hemorrhagic stroke was not analyzed due to few events. In Cohort 2, ischemic stroke (HR 0.41, CI 0.19–0.88) and hemorrhagic stroke (HR 034, CI 0.12–1.00) were lower in vegetarians.
In Cohort 1, lower stroke risk was seen only in vegetarians with low vitamin B12 intake, defined as < 2.4 μg per day (P=0.046). The researchers noted that vegetarians with low B12 intake consumed less animal protein (median 3 g vs 5 g) and were less likely to take B12 supplements (8.5% vs. 96%), making lower animal product intake a likely explanation for the association between lower stroke risk and lower B12 intake.
EPIC-Oxford: Ischemic Heart Disease and Stroke Incidence (2019)
A September 2019 report from the EPIC-Oxford study garnered much media attention. The study found that vegetarians had a 20% higher rate of total stroke than meat-eaters, equivalent to 3 more cases of total stroke per 1,000 people over a 10 year period, mostly due to a higher rate of hemorrhagic stroke (Tong, 2019). In this study, “vegetarians” included vegans (12.7% of the vegetarians).
The study also found that vegetarians had a 22% lower risk of ischemic heart disease than meat-eaters (a difference equivalent to 10 fewer cases of ischemic heart disease per 1,000 people over 10 years), which is in line with existing evidence. And vegetarians didn’t have a significantly higher risk of ischemic stroke than meat-eaters.
Hemorrhagic stroke is caused by bleeding in the brain, which is distinct from ischemic stroke, the more common type, which is caused by a blockage of blood flow to the brain.
A major risk factor for hemorrhagic stroke is high blood pressure, but vegetarians in this study had slightly lower blood pressure than meat-eaters. Research also suggests that low total and LDL cholesterol may increase the risk of hemorrhagic stroke (Ma, 2019, Wang, 2013, Valappil, 2012), and vegetarians had lower levels of both in this study.
Participants were separated into more specific dietary groups in the table below.
| Incidence of Cardiovascular Disease in EPIC-Oxford (2019) | |||||
|---|---|---|---|---|---|
| Meat-Eater | Pesco | Lacto-Ovo | Vegan | ||
| Number | 16,656 | 4,395 | 6,521 | 792 | |
| Heart Attack | 1.00 | 1.00 (.78-1.26) | .91 (.74-1.12) | .77 (.46-1.27) | |
| Ischemic Heart Disease | 1.00 | .87 (.77-.99) | .77 (.69-.86) | .82 (.64-1.05) | |
| Total Stroke | 1.00 | 1.14 (.94-1.38) | 1.17 (1.00-1.38) | 1.35 (.95-1.92) | |
| 18 years follow-up. Adjusted for age, sex, method of recruitment, region, year of recruitment, education, Townsend deprivation index, smoking, alcohol, physical activity, supplement use, oral contraception (women), hormone replacement therapy (women). Reference: Tong, 2019 |
|||||
AHS-2: Cardiovascular Mortality and Protein Source (2018)
In an analysis published in 2018, researchers found significantly higher rates of cardiovascular deaths associated with meat protein intake compared to nut and seed protein intake among a sample of 81,337 adults from the Adventist Health Study-2 (Tharrey, 2018). The multivariate-adjusted hazard ratios for cardiovascular mortality were 1.61 (98.75% CI, 1.12 2.32; P-trend <0.001) for the meat protein factor and 0.60 (98.75% CI, 0.42 0.86; P-trend <0.001) for the nuts and seeds protein factor (comparing highest versus lowest quintiles).
No significant associations were found for grains, legumes, fruits and vegetables, or processed foods. Researchers controlled for covariates including vegan diet, unsaturated fat, saturated fat, fiber, sodium, and antioxidant intake.
After accounting for these covariates, the association between cardiovascular deaths and type of protein remained statistically significant. Authors suggested there is something unique about the type of protein (such as amino acid composition), regardless of other dietary components, that impacts cardiovascular health.
Meta-Analysis of Mortality and Cancer (2017)
Dinu et al. (2017) compared vegans to omnivores for risk of all-cause mortality (RR: 0.88, 95% CI: 0.75 to 1.72) and cancer incidence (RR: 0.85, 95% CI: 0.75 to 0.95). Both findings were based on two prospective studies, EPIC-Oxford and AHS-2.
EPIC-Oxford: Mortality (2016)
In a 2016 report (Appleby, 2016), the mortality rate before age 90 in EPIC-Oxford was no different between vegetarians (including vegans) and regular meat-eaters (1.02, 0.94-1.10). Vegetarians had lower rates of mortality from pancreatic cancer (0.48, 0.28-0.82) and lymphatic cancer (0.50, 0.32-0.79). Semi-vegetarians had lower rates of death from pancreatic cancer (0.55, 0.36-.86). Pesco-vegetarians had lower death rates from all cancers (0.82, 0.70-0.97) but higher rates of cardiovascular disease (1.22, 1.02-1.46).
In the main analyses in the above paragraph, some participants were recategorized based on a change in their diets. The researchers did a second analysis in which participants who changed their diets were removed and found an 8% reduced risk of early death in vegetarians (0.92, 0.84-0.99). Limiting the results further, to deaths before age 75, strengthened the finding (0.86, 0.77-0.97).
When vegans were separated from other vegetarians, there were no statistically significant differences in mortality rates for the six large categories of death. Eliminating participants who had changed diet categories didn’t significantly change the results. The small number of deaths among vegans (166) as compared to the rest of the cohort (1,929) may have contributed to a lack of statistical significance.
EPIC-Oxford: Heart Disease Incidence (2013)
Heart disease rates of all vegetarians compared to all non-vegetarians were calculated for EPIC-Oxford from 1993 until 2009 (Crowe, 2013). These participants were all thought to be free of heart disease at the beginning of the study. The results showed that vegetarians had a statistically significant, ~30% reduced risk of heart disease. This finding held after adjusting for body mass index (BMI) and removing the first two years of follow-up.
The researchers believed the difference in heart disease rates to be due mainly to the lower non-HDL cholesterol levels and systolic blood pressure rates of the vegetarians.
| Risk of Heart Disease in Vegetarians Compared to Non-vegetarians in EPIC-Oxford (2013) | ||||
|---|---|---|---|---|
| Adjustments | Risk | |||
| Model One: age, smoking, alcohol, physical activity, education, socioeconomic status, oral contraceptives, hormone replacement therapy |
0.68 (0.58, 0.81) | |||
| Model One plus body mass index | 0.72 (0.61, 0.85) | |||
| Model One minus first 2 years of follow-up | 0.69 (0.58, 0.82) | |||
| Reference: Crowe, 2013 | ||||
AHS-2: Mortality (2013)
In 2013, death rates for the first 5.8 years of Adventist Health Study-2 were released (Orlich, 2013). Results are in the table below.
| Death Rates in Adventist Health Study-2 | |||||
|---|---|---|---|---|---|
| Meat-Eater | Semi-Veg | Pesco | Lacto-Ovo | Vegan | |
| Number | 35,359 | 4,031 | 7,194 | 21,177 | 5,548 |
| All Causes | 1.00 | .92 (.75-1.13) | .81 (.69-.94) | .91 (.82-1.00) | .85 (.73-1.01) |
| All Cardiovascular Disease | 1.00 | .85 (.63-1.16) | .80 (.62-1.03) | .90 (.76-1.06) | .91 (.71-1.16) |
| Ischemic Heart Disease | 1.00 | .92 (.57-1.51) | .65 (.43-.97) | .82 (.62-1.06) | .90 (.60-1.33) |
| Cancer | 1.00 | .94 (.66-1.35) | .94 (.72-1.22) | .90 (.75-1.09) | .92 (.68-1.24) |
| Other Causes | 1.00 | .99 (.72-1.36) | .71 (.54-.94) | .91 (.77-1.07) | .74 (.56-.99) |
| Adjusted for age, race, smoking, exercise, personal income, educational level, marital status, alcohol, region, sleep, sex, menopausal status, and hormone therapy. Further adjusting for body mass index and energy intake didn’t substantially impact results (data not shown). Reference: Orlich, 2013 |
|||||
Breaking the results down by sex indicated a significant benefit for cardiovascular disease for male vegans 0.58 (0.38-0.89) but not female vegans 1.18 (0.88-1.60). Analysis within the other causes category showed reductions in mortality from diabetes mellitus and renal failure for vegetarians.
Diet was measured at baseline and not re-assessed again (as distinct from EPIC-Oxford which measured diet numerous times during the study). The researchers believed that the short follow-up time of 5.8 years would bias the results towards finding no differences between diet groups.
In comparing their findings to British vegetarians, the researchers said:
The lack of similar findings in British vegetarians remains interesting, and this difference deserves careful study. In both cohorts, the non-vegetarians are a relatively healthy reference group. In both studies, the nutrient profiles of vegetarians differ in important ways from those of non-vegetarians, with vegetarians (especially vegans) consuming less saturated fat and more fiber. It appears that British vegetarians and US Adventist vegetarians eat somewhat differently. For instance, the vegetarians in our study consume more fiber and vitamin C than those of the EPIC-Oxford cohort: mean dietary fiber in EPIC-Oxford vegans was 27.7 g/d in men and 26.4 g/d in women compared with 45.6 g/d in men and 47.3 g/d in women in AHS-2 vegans; mean vitamin C in EPIC-Oxford vegans was 125 mg/d in men and 143 mg/d in women compared with 224 mg/d in men and 250 mg/d in women in AHS-2 vegans. Individuals electing vegetarian diets for ethical or environmental reasons may eat differently from those who choose vegetarian diets primarily for reasons of perceived superiority for health promotion. We believe that perceived healthfulness of vegetarian diets may be a major motivator of Adventist vegetarians.
Mortality Meta-Analysis (2012)
Although a 2012 meta-analysis by Huang et al. (Huang, 2012) is more recent, it may not be as reliable as the 1999 meta-analysis because it includes a study on Zen priests (Ogata, 1984) who were mostly semi-vegetarian and which used a standardized mortality ratio comparing all the Zen priests to the greater population rather than comparing the semi-vegetarians to the non-vegetarians within the same group. The Heidelberg Study results were also included and its comparison group were semi-vegetarians, which means there were semi-vegetarians in both the “vegetarian” and “non-vegetarian” groups in this meta-analysis. While not ideal, it should have biased the results against finding a beneficial effect of a vegetarian diet. In its favor, the 2012 meta-analysis includes data from EPIC-Oxford that wasn’t available for the 1999 meta-analysis.
| Meta-Analysis of Vegetarian Mortality (2012) | |||
|---|---|---|---|
| Mortality Rate of Vegetarians | |||
| All Causes | 0.91 (0.66, 1.16) | ||
| Ischemic Heart Disease | 0.71 (0.56, 0.87) | ||
| Cerebrovascular Disease (Stroke) | 0.88 (0.70, 1.06) | ||
| Combined Ischemic Heart and Circulatory Disease | 0.84 (0.54, 1.14) | ||
| Cancer Incidence | 0.82 (0.67, 0.97) | ||
| Reference: Huang, 2012 | |||
EPIC-Oxford: Heart Disease Mortality (2009)
After 10.7 years of follow-up, the results of death from heart disease, stroke, and all causes were released from EPIC-Oxford in 2009 (Key, 2009). There were no significant differences between vegetarians and meat-eaters for deaths from any of these diseases. This was likely due to the relatively few deaths from heart disease overall, not allowing for statistical power. The authors stated:
Average meat intake among the meat-eaters was only moderate, at 79 g/d in men and 67 g/d in women; these intakes are much lower than those reported in the National Diet and Nutrition Survey for the United Kingdom. Consumption of vegetables and fruit was higher among vegetarians than among non-vegetarians, but the differences were not large (< 20%). Thus, if high intakes of meat had an adverse effect and high intakes of fruit and vegetables had a beneficial effect, the relatively low meat intake and high fruit and vegetable intake of the non-vegetarians in this cohort could reduce the chance of observing lower mortality rates in the vegetarians than in the non-vegetarians.
Heidelberg Study (2005)
In 2005, results from 21 years of follow-up of the Heidelberg Study were published (Chang-Claude, 2005). The 1999 Meta-Analysis included 11 years of follow-up from this population.
There were only 60 vegans in the Heidelberg Study, which was 3% of the study group. The authors state, “Being a vegan was associated with a higher mortality risk (1.59; CI (confidence interval), 0.98-2.59) than being a lacto-ovo-vegetarian (1.08; CI, 0.86-1.34), when compared with non-vegetarians with moderate meat/ fish consumption, accounting for all other variables (data not shown).”
The “non-vegetarians” in the Heidelberg cohort were semi-vegetarians, eating very little meat. It’s likely that the vegans had a low rate of vitamin B12 supplementation.
Epic-Oxford: Preliminary Mortality Results (2003)
In 2003, preliminary results from EPIC-Oxford (Oxford component of the European Prospective Investigation into Cancer and Nutrition) comparing death rates of 46,562 subjects were reported (Key, 2003). About 33% of the subjects were vegetarian (including many vegans). The results showed no statistically significant differences between the vegetarians and non-vegetarians in any of the mortality categories which included cancer, circulatory disease, ischemic heart disease, cerebrovascular disease (stroke), all other causes, and all causes combined.
British Mortality (2002)
In 2002, the final death rate ratios were published from the Health Food Shoppers Study and the Oxford Vegetarian Study (Appleby, 2002). Because data on these populations have been published in the 1999 meta-analysis and many of the subjects went on to participate in EPIC-Oxford, I will not repeat the findings here.
However, there was one finding that has not been published elsewhere and it was the death rate ratio for “mental and neurological diseases.” The Health Food Shoppers Study showed no difference between vegetarians and non-vegetarians, but the Oxford Vegetarian study found vegetarians to have 2.5 times the number of deaths (2.46, 1.21-5.01). After excluding the first five years of follow-up, the death risk ratio went down to 2.21 (1.02 – 4.78). While the rate was statistically significant, and the difference was quite large, the confidence interval is very wide, indicating that it could possibly be due to random chance. Another likely explanation is that vitamin B12 deficiency was leading to neurological disorders. A less likely possibility, but one the that cannot be completely ruled out, is that vegetarians were suffering from low DHA levels.
Two analyses from the Adventist Health Study compared dementia in vegetarians to non-vegetarians, and were published in the same paper (Giem, 1993). The subjects had to have been vegetarian for at least 20 years. In the first, 68 vegans, 68 lacto-ovo vegetarians, and 136 omnivores were matched for age, gender, and zip code. The non-vegetarians were two to three times as likely to have dementia, though the finding was not statistically significant until previous meat-consumption was taken into account and even then it was just borderline. No difference in dementia was found between vegetarians and non-vegetarians among a second group of unmatched subjects. A 2013 report on mortality from Adventist Health Study-2 found no difference between vegetarians and non-vegetarians for death rates from neurologic diseases, though pesco- and semi-vegetarians were included in the “vegetarian” group (Orlich, 2013).
Based on the fact that Seventh-day Adventists have long been aware that vitamin B12 can’t be found in plants, and are a tight community with strong support for vegetarianism, vitamin B12 deficiency may have been less likely in the Adventist Health Study than in British vegetarians.
Mortality Meta-Analysis (1999)
A 1999 meta-analysis on vegetarian mortality used prospective data from the Adventist Mortality, Adventist Health, Oxford Vegetarian, and Heidelberg studies to compare mortality rates between types of vegetarians and non-vegetarians (Key, 1999). There weren’t many significant differences between diet groups, including none between the vegans and regular meat-eaters for any cause of death.
| Meta-Analysis of Vegetarian Mortality (1999) | |||||
|---|---|---|---|---|---|
| Meat-Eater | Semi-Veg | Pesco | Lacto-Ovo | Vegan | |
| Number | 31,766 | 8,135 | 2,375 | 23,265 | 753 |
| All Causes | 1.00 | .84 (.77-.90) | .82 (.77-.96) | .84 (.74-.96) | 1.00 (.70-1.44) |
| Ischemic Heart Disease | 1.00 | .80 (.69-.93) | .66 (.48-.90) | .66 (.52-.83) | .74 (.46-1.21) |
| Stroke | 1.00 | .97 (.75-1.25) | 1.04 (.65-1.64) | .87 (.66-1.13) | .70 (.25-1.98) |
| Colorectal Cancer | 1.00 | 1.14 (.72-1.82) | 1.00 (.42-2.38) | 1.10 (.79-1.54) | .83 (.11-6.17) |
| Breast Cancer | 1.00 | .97 (.56-1.71) | 1.50 (.74-3.04) | .75 (.49-1.14) | no cases |
| Prostate Cancer | 1.00 | 1.06 (.60-1.89) | 1.25 (.30-5.22) | .75 (.47-1.21) | no cases |
| Adjusted for age, sex, smoking status, and study. Reference: Key, 1999 |
|||||
Adventist Health Study (1999)
A 1999 report from the Adventist Health Study (Fraser, 1999) was the first major study of mortality rates of vegetarians in the USA. Table 4 shows the main results (except for cancer).
- Data collected from 1976-1988
- 34,192 participants, members of the Seventh-day Adventist church
- 29% were vegetarian; 7-10% of the vegetarians were vegan.
| Table 4. Adventist Health Study Results | ||||
|---|---|---|---|---|
| Men | Women | |||
| Vegetarians | Non-vegetarians | Vegetarians | Non-vegetarians | |
| BMIa | 24.3 | 26.2 | 23.7 | 25.9 |
| Heart disease | 38% Lower for Men | No Difference for Women | ||
| Overall mortality | Lived 3.21 more yrs | Lived 2.52 more yrs | ||
| aBMI—Body Mass Index. A measure of healthy body weight. Lower than 20 is underweight, while ≥ 25 is overweight. | ||||
Compared to the non-vegetarians, vegetarians had about:
- 1/2 the high blood pressure and diabetes
- 2/3 the rheumatoid arthritis
Life expectancies in the Adventist Health Study were published in 2001 (Fraser, 2001). They showed that white, non-Hispanic Seventh-day Adventists live longer than other white Californians (7.28 more years for men, 4.42 more years for women). According to the researchers, this group of Seventh-day Adventists was the longest-lived, formally studied population in the world (with an average lifespan of 78.5 years for men, 82.3 for women).
The following variables were shown to increase life expectancy:
- vegetarian diet
- eating nuts regularly
- physical activity
- lower body weight
- no smoking
Appendix A: Excluded Papers
The papers in this section aren’t included in the article above for various reasons.
Selinger et al.’s Umbrella Review of Meta-analyses (2023)
Selinger et al. (2023) published a meta-analysis of other meta-analyses looking at health outcomes of a vegan diet. Their report provided details of the primary studies included by the meta-analyses they compiled. But if there were no meta-analysis that included the most significant, primary studies on the subject, then those studies weren’t included.
For example, the prospective studies by Tonstad et al. (2013) and Papier et al. (2019) didn’t make it into Selinger et al.’s report, thus leading to a weakened benefit of the risk of diabetes for vegans. Appleby et al.’s (2002) study reporting lower rates of hypertension among vegans also didn’t make it into Selinger et al.’s analysis.


6 thoughts on “Mortality and Cardiovascular Disease Rates of Vegetarians”
I am so confused. Some of these show higher mortality rates others don’t? Is this healthy or not?
Sorry, I should probably add a summary at the top of the article so people don’t have to read the details. Overall, there’s a strong case that vegetarians (including vegans) don’t have a significant difference in mortality rates between regular meat-eaters, other things being equal. Vegetarians (including vegans) appear to have a lower incidence of heart disease and vegans, especially, have a lower incidence of type 2 diabetes. This means that vegetarians are probably healthier while alive, but don’t necessarily live longer.
You link the (excellent) veganrd.com on your website. One article there, ‘Why some people fail at being vegan’, refers to the US Human Research Council study of 11k US citizens. It was found that 12% are or had at one time been vegan. Of these, 70% had given up their plant-based diet. It seems to be that about 45% of the ‘gave-uppers’ did so because they felt unwell and many of them felt better on returning to being omnivorous. Turning to the statistics you quote for vegan longevity, you conclude as follows: ‘In summary, not enough is yet known about vegan mortality to draw any conclusions other than that vegans do not have unusually high rates of mortality and they probably do better than the average person due either to diet or a healthier lifestyle’. Is it not the case that these statistics measure those vegans that have felt healthy and thus persisted with the diet, but they exclude the 45% who felt unwell and gave up. Can it not be said, therefore, that the results are greatly skewed? The ‘vegan unwell’ jumped ship while the ‘vegan well’ got into the mortality statistics, giving a favourable bias to the results. Therefore, in no way can it be said that vegans live as long omnivores. It can only be said that it appears that vegans who feel well on a plant-based diet live as long as omnivores.
Nigel,
The Humane Research Council study on vegetarian recidivism was a cross-sectional study and had no limit on the length of time someone had to be vegetarian (or vegan) before they could qualify as an ex-vegetarian. In other words, if someone considered themselves to follow a vegetarian diet for one day, they would have qualified to be an ex-vegetarian for the survey.
On the other hand, cohort studies measuring disease rates in vegetarians are prospective studies that follow people through time and measure their disease outcomes. They usually require that someone be a vegetarian for some period of time. For example, the EPIC-Oxford study participants were given follow-up surveys approximately 5, 10, and 15 years after entering the study to verify their diet.
The authors state, “When we excluded data for participants known to have changed diet group at least once during follow-up, leaving data for 4270 deaths before age 90, there was no significant difference in risk between diet groups for all causes of death combined, as follows: low meat eaters, HR: 0.93 (95% CI: 0.85, 1.02); fish eaters, HR: 0.91 (95% CI: 0.81, 1.02); and vegetarians and vegans, HR: 0.92 (95% CI: 0.84, 0.99) compared with regular meat eaters.” They don’t indicate how many people went from meat-eater to fish-eater to vegetarian, or the other direction, or whether they tested to see if one direction impacted the results more than another.
The Vegetarian Resource Group conducted a prospective study among their members and found a high retention rate among those completing the follow-up survey, including, “One hundred percent of vegan males stayed vegan, while 83% of females stayed vegan.” We don’t know how well that extrapolates to other vegetarians, but it’s a stark contrast to the Humane Research Council’s study and used an arguably better methodology for determining recidivism rates (i.e., prospective instead of cross-sectional and based on people who presumably had some resolve in being vegetarian).
“Based on the fact that Seventh-day Adventists have long been aware that vitamin B12 cannot be found in animal (??? maybe NON-ANIMAL? or PLANT?) products and are a tight community with strong support for vegetarianism, it seems likely that vitamin B12 deficiency would be less likely in the Adventist Health Study than in British vegetarians.”
Nikita,
Good catch, it’s fixed. Thanks.