Contents
- Introduction
- B12 Functions
- Homocysteine Clearance
- Anemia, DNA, and Folate
- Lack of Anemia Does Not Mean B12 Status Is Healthy
- Methylmalonic Acid (MMA)
- References
Introduction
Eussen et al. (3) summarize vitamin B12’s functions in humans:
Vitamin B-12 is involved in one-carbon metabolism, during which it plays a role in the transfer of methyl groups and methylation reactions that are important for the synthesis and metabolism of neurotransmitters and phospholipids in the central nervous system. Moreover, vitamin B-12 is required for nucleic acid synthesis and hematopoiesis and for the metabolism of fatty acids and amino acids in the mitochondrial citric acid cycle. In addition to causing anemia, vitamin B-12 deficiency has been linked with several neurologic disorders, such as neuropathy, myelopathy, dementia, depression, memory impairment, and cerebrovascular disease. Although prolonged vitamin B-12 deficiency may eventually result in irreversible neurologic damage and cognitive impairment, early stages of vitamin B-12 deficiency—detected by elevated concentrations of plasma total homocysteine and methylmalonic acid and decreased concentrations of holotranscobalamin—may result in milder forms of cognitive impairment in the absence of anemia.
B12 Functions
In the cells of mammals (1), there are two different co-enzyme forms of vitamin B12 (2):
- Methylcobalamin
- Used by the enzyme methionine synthase to turn homocysteine into methionine. Methionine is further converted to the important methyl donor, S-adenosylmethionine (SAM, aka SAMe)
- 5′-deoxyadenosylcobalamin
- Used by the enzyme methylmalonyl-CoA mutase to convert methylmalonyl-CoA to succinyl-CoA
Homocysteine Clearance
Methionine is an essential amino acid provided by the diet. Some methionine is turned into homocysteine and without adequate vitamin B12, homocysteine builds up in the blood. Although it’s not clearly a causative factor, elevated homocysteine is associated with early death, cardiovascular disease, and dementia. For more information, see Homocysteine and Mild B12 Deficiency in Vegans.
Anemia, DNA, and Folate
Traditionally, B12 deficiency, normally resulting from the inablity to absorb B12, was diagnosed by finding abnormally large red blood cells. This sort of anemia has two names:
- Macrocytic anemia – above normal mean corpuscular volume (MCV)
- Megaloblastic anemia – abnormally large red blood cells observed under a microscope
The vitamin folate (aka folic acid) affects the anemia symptoms of B12 deficiency. Folate is needed to turn uracil into thymidine, an essential building block of DNA (4). DNA is needed for new red blood cell production and division. B12 is involved in this process because in creating methylcobalamin (used in the homocysteine to methionine reaction), B12 produces a form of folate needed to make DNA. If there is no B12 available, this form of folate can become depleted (known as the methyl-folate trap) and DNA production slows (5). See the pathway below.
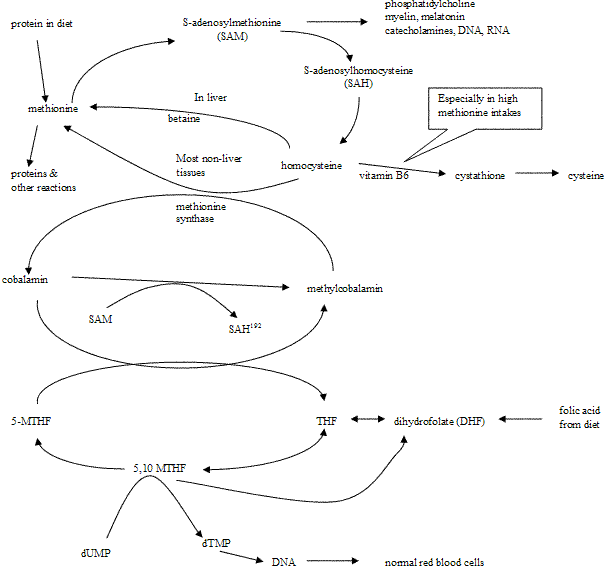
Only RNA is needed to produce the hemoglobin found in the red blood cells. Unlike DNA, RNA does not require thymidine. Therefore, if there is not adequate folate, the new red blood cells (which start out as large cells called reticulocytes) divide slowly, as they are dependent on DNA for dividing. At the same time, their hemoglobin is only dependent on RNA and it is produced at a normal rate. This causes large red blood cells known as macrocytes (4, 6). If enough of these macrocytes accumulate, the result is macrocytic anemia.
If there are large amounts of incoming folate from the diet, the body does not need to rely on the regeneration of folate from the B12 cycle. Instead, it can use the extra dietary folate to produce DNA, thus preventing macrocytic anemia (see the bottom right-hand portion of Figure 1 above). This is why high intakes of folate are said to “mask” a B12 deficiency.
To complicate things further, an iron deficiency results in small red blood cells from inadequate hemoglobin synthesis and can counteract abnormally large red blood cells making it appear as though blood cell size is normal when there are multiple nutritional deficiencies (7).
Intestinal cells are also rapidly dying and being replaced using DNA. A B12 deficiency can make itself worse because it can prevent the production of the intestinal cells needed to absorb B12.
Lack of Anemia Does Not Mean B12 Status Is Healthy
Traditionally, the existence of macrocytic anemia was relied on to indicate a B12 deficiency. However, neurological disorders due to B12 deficiency commonly occur in the absence of a macrocytic anemia.
Lindenbaum et al. (8) (1988, USA) examined 141 cases of neurological problems due to B12 deficiency. 40 (28%) had no macrocytic anemia (iron deficiency may have contributed to a lack in 6 patients, and folate therapy could account for 2 others). These 40 had very high serum MMA levels (range: .76-187 µmol/l, 78% > 2 µmol/l) and homocysteine levels (23-289 µmol/l, 45% > 100 µmol/l). Characteristic features of patients with B12 deficiency but without macrocytic anemia included: sensory loss, inability to move muscles smoothly (ataxia), dementia, and psychiatric disorders. They also had borderline (and sometimes normal) B12 levels (see Table 1). One patient died during the first week of treatment, but the other 39 benefited from B12 therapy. Some patients had residual abnormalities after years of treatment.
| Table 1. B12 Levels in Neurological Patients Without Macrocytic Anemia (pg/ml) | |
|---|---|
| Number of Patients | Serum B12 |
| 2 | > 200 |
| 16 | 100-200 |
| 22 | < 100 |
In a 2011 study from Korea, among 35 patients with vitamin B12 deficiency, most of whom had neurological symptoms, none had anemia (12).
Methylmalonic Acid (MMA)
The second coenzyme form of B12, adenosylcobalamin, takes part in the conversion of methylmalonyl-CoA to succinyl-CoA. When B12 is not available, methylmalonyl-CoA levels increase. Methylmalonyl-CoA is then converted to methylmalonic acid (MMA) which then accumulates in the blood and urine. Since B12 is the only coenzyme required in this pathway, MMA levels are the best indicators of a B12 deficiency.
Elevated MMA levels can also be caused by genetic defects, kidney failure, low blood volume, gut bacteria changes, pregnancy, and thyroid disease (9, 10).
For more information on elevated methylmalonic acid, see Minimizing Methylmalonic Acid Levels.
References
1. Scalabrino G. Subacute combined degeneration one century later. The neurotrophic action of cobalamin (vitamin B12) revisited. J Neuropathol Exp Neurol. 2001 Feb;60(2):109-20.
2. Seetharam B, Li N. Transcobalamin II and its cell surface receptor. Vitam Horm. 2000;59:337-66.
3. Eussen SJ, de Groot LC, Joosten LW, et al. Effect of oral vitamin B-12 with or without folic acid on cognitive function in older people with mild vitamin B-12 deficiency: a randomized, placebo-controlled trial. Am J Clin Nutr. 2006;84(2):361-370.
4. Guyton AC, Hall JE. Textbook of Medical Physiology, 9th ed. Philadelphia, PA: W.B. Saunders, Co: 1996. p. 845-7.
5. Murray RK, Granner DK, Mayes PA, Rodwell VW. Harper’s Biochemistry, 24th ed. Appleton & Lange, 1996.
6. Groff J, Gropper S. Advanced Nutrition and Human Metabolism, 3rd ed. Wadsworth: 2000.
7. Herbert V. The 1986 Herman Award Lecture. Nutrition science as a continually unfolding story: the folate and vitamin B-12 paradigm. Am J Clin Nutr. 1987;46:387-402.
8. Lindenbaum J, Healton EB, Savage DG, Brust JC, Garrett TJ, Podell ER, Marcell PD, Stabler SP, Allen RH. Neuropsychiatric disorders caused by cobalamin deficiency in the absence of anemia or macrocytosis. N Engl J Med. 1988 Jun 30;318(26):1720-8.
9. Minet JC, Bisse E, Aebischer CP, Beil A, Wieland H, Lutschg J. Assessment of vitamin B-12, folate, and vitamin B-6 status and relation to sulfur amino acid metabolism in neonates. Am J Clin Nutr. 2000 Sep;72(3):751-7.
12. Kim HI, Hyung WJ, Song KJ, Choi SH, Kim CB, Noh SH. Oral vitamin B12 replacement: an effective treatment for vitamin B12 deficiency after total gastrectomy in gastric cancer patients. Ann Surg Oncol. 2011 Dec;18(13):3711-7.
13. References for Figure 1: Vitamin B12 Cycle
Fenech M. Micronucleus frequency in human lymphocytes is related to plasma vitamin B12 and homocysteine. Mutat Res. 1999 Jul 16;428(1-2):299-304.
Groff J, Gropper S. Advanced Nutrition and Human Metabolism, 3rd ed. Wadsworth: 2000.
Herrmann W, Schorr H, Purschwitz K, Rassoul F, Richter V. Total homocysteine, vitamin b(12), and total antioxidant status in vegetarians. Clin Chem. 2001 Jun;47(6):1094-101.
Kirke PN, Molloy AM, Daly LE, Burke H, Weir DG, Scott JM. Maternal plasma folate and vitamin B12 are independent risk factors for neural tube defects. Q J Med. 1993 Nov;86(11):703-8.
Krajcovicova-Kudlackova M, Blazicek P, Kopcova J, Bederova A, Babinska K. Homocysteine levels in vegetarians versus omnivores. Ann Nutr Metab. 2000;44(3):135-8.
Loehrer FM, Schwab R, Angst CP, Haefeli WE, Fowler B. Influence of oral S-adenosylmethionine on plasma 5-methyltetrahydrofolate, S-adenosylhomocysteine, homocysteine and methionine in healthy humans. J Pharmacol Exp Ther. 1997 Aug;282(2):845-50.
Refsum H. Folate, vitamin B12 and homocysteine in relation to birth defects and pregnancy outcome. Br J Nutr. 2001 May;85 Suppl 2:S109-13.
Selhub J, Bagley LC, Miller J, Rosenberg IH. B vitamins, homocysteine, and neurocognitive function in the elderly. Am J Clin Nutr. 2000 Feb;71(2):614S-620S.

2 thoughts on “Vitamin B12 Coenzyme Functions”
What does the s in sMMA stand for?
Eddie,
sMMA stands for serum MMA (i.e., MMA levels in blood serum). Based on your question, I replaced all the sMMA with serum MMA to prevent confusion.