by Jack Norris, RD
[Correction (February 21, 2021):
A reader pointed out that in the iodine section, I said, “The only significant association between subclinical hypothyroidism and bone mineral density (BMD) was an increased BMD in the higher femur neck in women.” I then conclude the section with “Given that 1) hip and leg fractures played a large role in the higher fracture rate among vegans in EPIC-Oxford, 2) subclinical hypothyroidism is associated with lower BMD in the femur [emphasis added], and 3) U.K. vegans have questionable iodine status, it seems possible that iodine deficiency could contribute to their higher fracture rate.”
When I wrote the final summary of the iodine section, I misread the finding for femur BMD, forgetting that the result had been counterintuitive. I’ve now updated my assessment that iodine deficiency could contribute to the fracture rates of vegans from “possible” to “unlikely.” I’m sorry for that mistake.]
Entire article is Bone Fractures among U.K. Vegans: Implications and Recommendations.
In Part 3 below:
- Zinc
- Iodine
- Selenium
Zinc
Zinc is both a component of bone and also involved in many metabolic pathways that could impact bone health. The DRI for zinc is 11 mg for men and 9 mg for women. Vegans typically ingest close to the DRI through food, but there’s a concern that lower zinc absorption from plant foods could interfere with many vegans reaching optimal zinc status.
Studying the relationship between zinc intake and disease is complicated by the fact that zinc comes in high-protein foods and often in conjunction with a number of other minerals. There’s also no easy way to assess zinc status.
A 2021 meta-analysis of 40 studies examined associations between zinc intakes (both from food and supplements), serum zinc levels, bone mineral density and markers, and fracture risk (Ceylan, 2021). Low serum zinc levels were associated with a higher rate of osteoporosis among case-control studies. Caloric intake and zinc intake from supplements, but not from food, were associated with higher serum zinc levels. Zinc supplementation appeared to be associated with higher BMD at the femoral neck but lower BMD in the lumbar spine. Figure 6 of Ceylan et al. shows higher BMD in the lumbar spine and femur was associated with a serum zinc level of about 80 to 90 µg/dl.
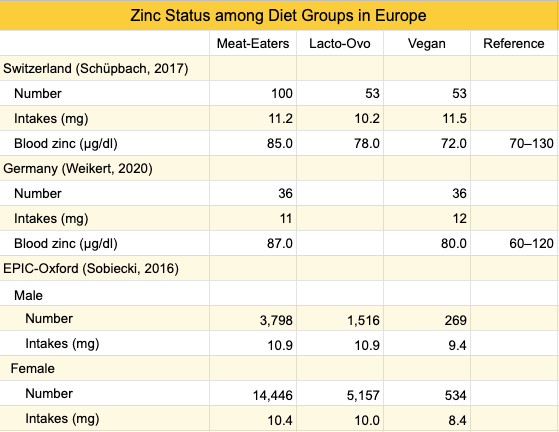
The table below shows the zinc levels and intakes of vegans compared to meat-eaters and lacto-ovo-vegetarians in three studies, including from the EPIC-Oxford survey conducted in 2010.
The vegans in EPIC-Oxford had zinc intakes lower than the vegans in the studies from Switzerland and Germany, and the vegans from Switzerland and Germany had lower serum zinc levels than those associated with higher bone mineral density in Ceylon et al. This suggests that poor zinc status might have impacted bone health among vegans in EPIC-Oxford.
Vegans should make an effort to include foods high in zinc or take a multivitamin or modest zinc supplement. See Daily Needs for recommendations.
Iodine
Lightowler and Davies (1998) found a urinary iodine concentration (UIC) for vegans in the U.K. well below what’s considered healthy for a population, and the second-lowest average vegan UIC recorded to date. However, there are problems in using UIC to assess the iodine status of vegans (see Urinary Iodine Concentrations of Vegans). Through chemical analysis, Lightowler found baseline iodine intakes from food to be 87 µg/day which, while far short of the RDA of 150 µg/day, approximates the mean daily iodine turnover of ~95 µg/day (Zimmermann, 2012). Dietary iodine is absorbed at a rate of >92% (Zimmermann, 2012), leaving these UK vegans with a slightly lower intake, on average, than required for iodine turnover unless they were taking supplements. Key et al. (1992) found mostly normal thyroid hormone levels among vegan men from the U.K., with the notable exception being vegans who were likely receiving excessive iodine by supplementing with kelp. It’s noteworthy that vegans supplementing with kelp in Key et al. had hypothyroidism rather than hyperthyroidism.
A meta-analysis of subclinical thyroid dysfunction examined data from 17 cohort studies (Zhu, 2020). Subclinical hypothyroidism was not associated with an increased risk of any fracture (P = 0.166), hip fracture (P = 0.068), or spine fracture (P = 0.818). The only significant association between subclinical hypothyroidism and bone mineral density (BMD) was an increased BMD in the higher femur neck in women. In contrast, subclinical hyperthyroidism (not hypo-) was associated with an increased risk of fracture (RR 1.17, CI 1.08–1.26).
Given that 1) hip and leg fractures played a large role in the higher fracture rate among vegans in EPIC-Oxford, 2) subclinical hypothyroidism is associated with lower BMD in the femur, and 3) U.K. vegans have questionable iodine status, it seems possible that iodine deficiency could contribute to their higher fracture rate. Given that there isn’t an association between subclinical hypothyroidism and increased fracture rates in the general population and that while vegans in the United Kingdom might have low iodine intakes they still appear to have normal thyroid hormone levels, it seems unlikely that iodine could have played much of a role in the higher fracture rates found among vegans in EPIC-Oxford. It’s still prudent for vegans to make sure they have a reliable source of iodine (see Daily Needs).
Selenium
In a prospective study from the U.K. of 1,144 postmenopausal women, higher selenium levels were associated with greater bone mineral density at the hip, but not the lumbar spine, at study entry but not after 6 years of follow-up (Hoeg, 2012). There was also no association between selenium levels and bone fractures after 6 years of follow-up.
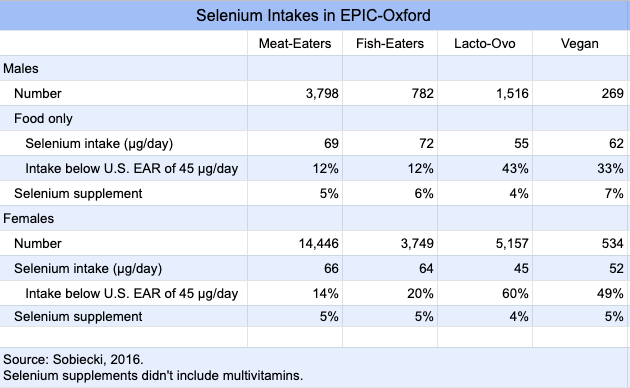
In EPIC-Oxford, a follow-up survey sent to participants an average of 14.3 years after recruitment, found that a high percentage of vegetarians weren’t meeting the estimated average requirement (EAR) for selenium (Sobiecki, 2016).
In the case of EPIC-Oxford, vegans had higher selenium intakes than lacto-ovo-vegetarians, whereas lacto-ovo-vegetarians had total fracture rates similar to meat-eaters (HR 1.07, CI 0.97-1.18). If selenium was increasing the fracture rates of vegans, it seems like it should be doing the same for lacto-ovo-vegetarians.
In contrast to selenium intakes being higher for vegans than lacto-ovo-vegetarians in EPIC-Oxford, selenium levels in toenails from the U.K. county of Norfolk showed significantly different selenium levels between omnivores (685 ng/g, n=67), lacto-ovo-vegetarians (591 ng/g, n=23), and vegans (541 ng/g, n=34). The authors reported that Norfolk’s soil is high in selenium (Judd, 1997).
A cross-sectional study from Germany comparing 36 sex and age-matched omnivores and vegans found no significant difference between median plasma selenium levels: 77 µg/l vs. 68 µg/l, respectively (Weikert, 2020). However, there was a significant difference in selenoprotein P levels which are more indicative of selenium status (omnivores: 5.0 mg/l; vegans: 3.3 mg/l). No reference range was provided and selenium intakes weren’t measured.
In comparing the German vegans in Weikert et al. to the quintiles of women with higher bone mineral density in Hoeg et al., the vegans would have had low selenium plasma levels but adequate selenoprotein P levels.
While it’s unlikely that poor selenium status explains a significant portion of the higher fracture rate in EPIC-Oxford, because selenium intakes can be low in vegan diets in some countries, it’s important that vegans in those countries ensure an adequate source (see Selenium).
Coming up in Part 4:
- Vitamin D
- Calcium
- Protein
References